The Business Case for Clinical Intelligence in the ICU. Is it a Worthwhile Investment?
Blog
Hospital operating margins remain thin and ICU cost is one of the largest line items in any high-acuity hospital. Clinical intelligence software, used as adjunctive support for clinician-directed care, has been associated with shorter ICU length of stay, fewer unplanned readmissions, and reduced ventilation time. Despite this, many senior hospital leaders are unsure of the impact of clinical intelligence software. This blog examines whether it’s a worthwhile investment and explores its potential.
Why the ICU drives hospital margin
ICU beds make up roughly 12% of staffed hospital beds in the United States but are estimated to consume a disproportionately large share of total hospital costs1. Modest operational improvements inside the ICU therefore have an outsized effect on a hospital’s P&L. Unfortunately, hospital expense growth continues to outpace reimbursement and median operating margins now sit in low single digits2. Leaders are being asked to find value without adding capacity, which puts operational improvement inside high-cost ICU units at the top of the priority list.
Clinical intelligence in critical care: from promise to operational use
A 2024 review surveyed the evolving role of AI across acute and intensive care, from emergency dispatch and triage through to documentation, imaging, and ICU decision support3. It reported that AI-driven triage models have surpassed human performance in retrospective studies and concluded that AI’s potential to streamline clinical workflows is now evident. For hospital decision-makers, clinical intelligence software sits firmly inside the mainstream of credible critical care medicine, not at its experimental edge.
How the Etiometry clinical intelligence platform delivers ICU ROI
Etiometry provides adjunctive insight to support clinician-directed, personalized escalation and de-escalation decisions within hospital-defined workflows. The platform holds 11 FDA clearances, more than any other clinical intelligence software platform, and was developed from more than 150 million hours of de-identified patient data.
Three published outcome studies illustrate the financial levers available.
- Shorter ICU length of stay. Use of the Etiometry platform, evaluated using causal-inference methods against a 21-hospital registry control group, was associated with an 18% reduction in postoperative ICU length of stay4.
- Fewer unplanned readmissions. The same multi-centre analysis reported a 41% reduction in unplanned ICU readmissions, a direct lever against HRRP penalty exposure.
- Reduced ventilation time. A platform-supported spontaneous breathing trial review workflow was associated with a 30% reduction in mechanical ventilation time and a 20% reduction in overall hospital length of stay in an observational pediatric cardiac surgery study5.
The Automated Spontaneous Breathing Trial Performance Tool study also helps us to understand the specific cost savings available from a reduction in post operative LOS and mechanical ventilation time. When risk-adjusted and translated into hospital cost terms, these improvements equate to estimated savings of between $3,672 and $9,391 per patient. With the average inpatient day costing around $2,623 and each additional day of mechanical ventilation adding roughly $1,500, even modest reductions in length of stay can rapidly deliver substantial financial benefit across a hospital’s annual case volume.
How clinical outcome improvements translate into reduced ICU cost of care
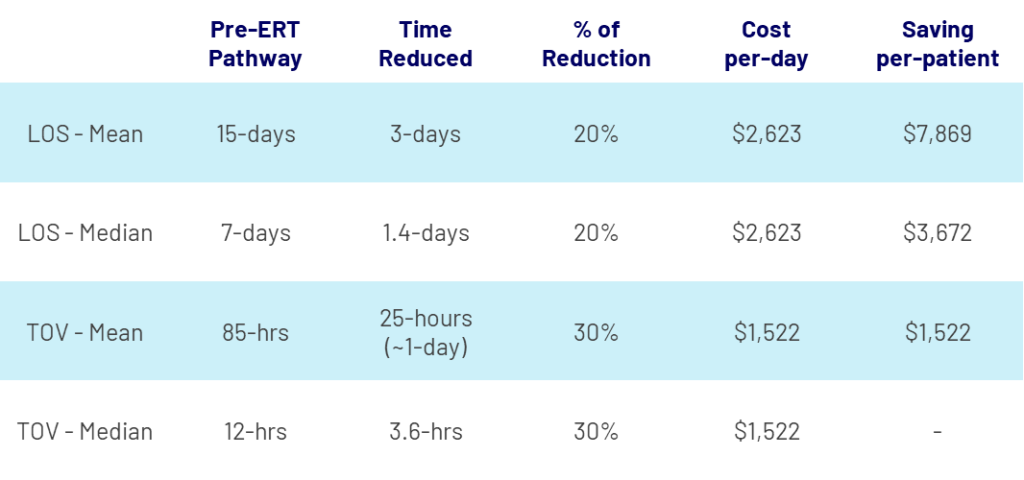
Assumptions
- Cost per day: $2,623
Source: https://www.statista.com/statistics/630443/inpatient-day-hospital-costs-in-us-by-nonprofit-or-profit/ - Mean incremental cost of mechanical ventilation in intensive care unit patients: $1,522 dollars per-day
Conclusion
Clinical intelligence is not an experiment. Used as adjunctive support inside hospital-defined workflows, it is associated with shorter ICU stays, fewer readmissions, and less ventilator time, each of which translates into freed capacity, avoided penalties, and protected margin. For health systems facing 2026 margin pressure, the business case for clinical intelligence in the ICU is no longer speculative.
Request a Demo
Frequently Asked Questions
What is the typical payback period for clinical intelligence software in the ICU?
Payback is driven by various outcome improvements such as length of stay reductions, readmission avoidance, and ventilation time. Actual payback depends on case mix, ICU volume, and contracted use.
How can clinical intelligence reduce HRRP penalty exposure?
By providing adjunctive insight to support clinician-directed, personalized decisions, clinical intelligence can support earlier clinician review and protocolised de-escalation. In one multi-centre causal-inference analysis of the Etiometry platform, unplanned ICU readmissions fell by 41%, a potential impact on CMS Hospital Readmissions Reduction Program exposure.
How does Etiometry fit alongside an existing Epic or Cerner EHR?
Etiometry sits as an adjunctive layer above the EHR. It organizes live physiologic data from monitors, ventilators, labs, and other medical devices into one patient view and provides FDA-cleared risk indices for clinician-directed escalation and de-escalation decisions. The EHR remains the system of record.
Resources
- Society of Critical Care Medicine. Critical Care Statistics. Available at: https://sccm.org/communications/critical-care-statistics
- American Hospital Association. 2025 Cost of Caring Report. March 2026. Available at: https://www.aha.org/guides-and-reports/2026-03-09-2025-cost-caring-report
- Biesheuvel LA, Dongelmans DA, Elbers PWG. Artificial intelligence to advance acute and intensive care medicine. Current Opinion in Critical Care. 2024;30(3):246-250. Available at: https://journals.lww.com/co-criticalcare/fulltext/2024/06000/artificial_intelligence_to_advance_acute_and.10.aspx
- Gaies M et al. Methods to Enhance Causal Inference for Assessing Impact of Clinical Informatics Platform Implementation. Circulation: Cardiovascular Quality and Outcomes. 2023. Available at: https://www.ahajournals.org/doi/10.1161/CIRCOUTCOMES.122.009277
- Borasino S et al. Automated Spontaneous Breathing Trial Performance Tool is Associated with Improved Outcomes Following Pediatric Cardiac Surgery. Journal of Pediatric Critical Care. 2025. Available at: https://journals.lww.com/jpcr/fulltext/2025/01000/automated_spontaneous_breathing_trial_performance.1.aspx


